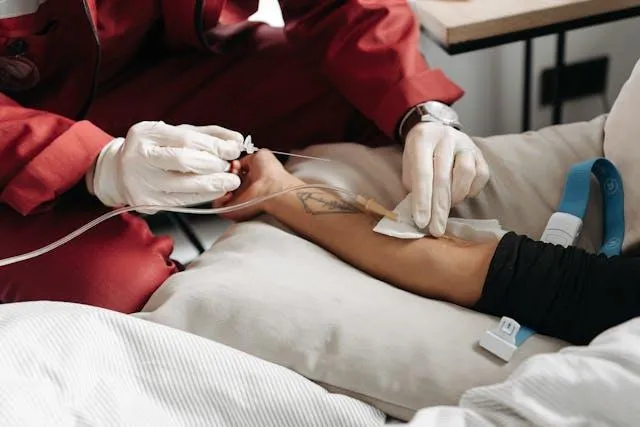
Dignity SA defined assisted dying as a medically-assisted death that can be either self-administered or administered by a doctor, governed strictly by eligibility criteria and robust safeguards.
Image: Pavel Danilyuk/Pexels
DIGNITY SA has taken a bold step by filing a court application to declare the prohibition of assisted dying or euthanasia unconstitutional, advocating for the right to a dignified death for those suffering from terminal conditions in South Africa.
The application was lodged at the North Gauteng High Court in Pretoria after a 15-year fight for the decriminalisation of medically-assisted dying.
Dignity SA made the application against the minister of justice and constitutional development, the national director of public prosecutions (NDPP), the Minister of Health Dr Aaron Motsoaledi, and the Health Professions Council of South Africa (HPCSA) last week.
It argued that the current common-law prohibition of assisted dying was “unconstitutional and invalid”, and that South Africans should have a right to choose a “dignified end when facing intractable and unbearable suffering”.
Dignity SA defined assisted dying as a medically-assisted death that can be either self-administered or administered by a doctor, governed strictly by eligibility criteria and robust safeguards.
In its application, Willem Landman, the organisation’s founder, said the application was brought to court on behalf of all people with terminal or irremediable conditions, and who are suffering intolerably, and wished to exercise the choice of medically-assisted dying.
He said the application was also on behalf of practitioners who considered that they ought to be able to alleviate a patient's suffering in accordance with the latter’s choice, free from the risk of criminal or professional sanctions
“It is currently illegal, in terms of the criminal branch of the common law, for a health practitioner to provide medical assistance in dying to a patient. The HPCSA guidelines also classify the provision of medical assistance in dying by health practitioners as unethical and unprofessional conduct.
“Dignity SA submits that individuals with a terminal or irremedial condition have a constitutional right, in appropriate circumstances, to ask for and be afforded medical assistance in dying.
“It accepts that the exercise of the right must be properly controlled. It is not the purpose of this application to design controls. That is to be left to Parliament.
“Medical assistance in dying should only be afforded to qualified patients who suffer a terminal or irremediable condition, whose suffering is unbearable or intolerable, who are capable of making an informed request for medical assistance in dying, and who make an informed voluntary and considered request for medical assistance in dying,” Landman added.
He said only registered health professionals should be allowed to render medical assistance in dying.
“Medical assistance in dying may, in a wide sense, refer to a number of end-of-life interventions, including assistance with terminal pain management (including palliative sedation); withholding or withdrawal of potentially life-sustaining treatment – including artificial nutrition and hydration; issuing do-not-rescusitate orders; and respecting living wills or other advance directives.
“The current law is that practitioner-administered medical assistance in dying constitutes the crime of murder on the part of the health practitioner. There is no allowance in the criminal law for a person to request or to consent to being actively killed by another
“Euthanasia is the employment of any medical intervention primarily aimed at ending a patient's life by giving a patient a lethal drug or injection. At present, South African courts have acknowledged that both euthanasia and doctor-assisted suicide are fundamentally incompatible with a practitioner's role as a healer and a practitioner guilty of either is regarded as having acted unethically and unlawfully.
“The Health Professions Act empowers the HPCSA and professional boards established under the act to take disciplinary steps against health practitioners who are said to have participated in “unprofessional conduct” or improper or disgraceful conduct.
“The approach of the HPCSA deems medically-assisted dying as unethical and unlawful, placing medical assistance in dying in the realm of unprofessional and improper conduct, with the result that health practitioners who provide medical assistance in dying face consequences, risk of unethical practices and murder charges, and their licences revoked.
“In our constitutional dispensation, I am advised that courts cannot shy away from difficult topics, or abdicate their duty to pronounce on matters affecting fundamental rights.
The right to put an end to intolerable suffering, to regain control over one’s body, and to die with dignity is a matter which the courts can no longer avoid,” he added.
Landman said in the organisation's 15-year fight to have medically-assisted dying decriminalised, Dignity SA has received more than 150 requests for information about or advice on euthanasia.
“For a number of them, however, the prohibition on medically-assisted dying meant that they were not able to be assisted by a health practitioner to ensure a safe and peaceful death. For others, it meant that they had to hide their death from their family and friends, being alone in their final moments, and for others it meant that they died knowing that in acting out their wishes, there may well be criminal consequences for the person who assisted them,” he added.
He said the submission was supported by expert reports of Professor Graham Fieggen, head of neurosurgery at the University of Cape Town, and Professor Keymanthri Moodley, a bioethicist with 25 years of experience.
He said both professors had attested that the country’s medical profession would be capable of implementing medical assistance in dying.
“Moodley’s report emphasises that the country’s healthcare professionals routinely make complex end-of-life decisions involving withdrawal of treatment, particularly in intensive care and oncology settings.
“Both Fieggen and Moodley highlight that South Africa already operates sophisticated safeguards systems in analogous high-stakes and complex medical contexts, including organ transplantation, renal dialysis allocation, and termination of pregnancy services. These existing regimes demonstrate the healthcare systems capacity to implement eligibility criteria, multipractitioner assessments, and robust oversight mechanisms that would be essential for the provision of medically-assisted dying.
“The reports recommend a hospital co-ordinated implementation model, initially operating through accredited secondary and tertiary hospitals with established multidisciplinary teams, palliative care services, and ethics committees,” Landman said in the application.
Related Topics: